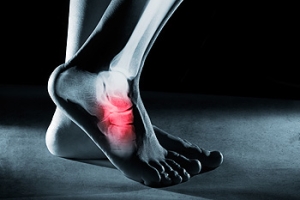
The Causes, Types, and Treatments of Achilles Tendon Injuries
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
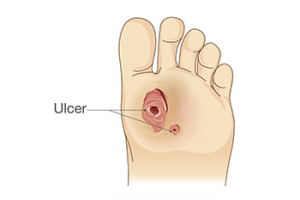
What Are Diabetic Foot Ulcers?
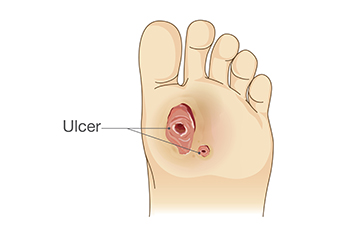
Diabetic foot ulcers are serious complications of diabetes, characterized by open sores or wounds that typically develop on the feet. They result from poor circulation, nerve damage, also called neuropathy, and impaired immune function associated with diabetes. Treatment involves meticulous wound care, which includes cleaning the ulcer with gentle soap and water, applying antibiotic ointment, and covering it with a sterile dressing. Offloading pressure from the affected foot is important to prevent further irritation and aid healing. Podiatrists can conduct regular exams to monitor ulcers, assess circulation, and provide guidance on footwear and hygiene. Timely intervention can prevent complications such as infections or amputations. If you have diabetes, it is strongly suggested you visit a podiatrist who can help you to manage this condition.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with John McGhan, DPM from Gold Canyon Foot & Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Gold Canyon, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
The Hidden Dangers of Flip-Flops on Your Feet
 Flip-flops, though convenient, can be harsh on your feet, especially for individuals at risk like those with diabetes. The lack of support in flip-flops leads to improper heel strike, causing stress on the heels and increasing the risk of plantar fasciitis. Further, to keep the flip flops on, wearers often grip with their toes, which can cause muscle strain and negatively affect conditions like hammertoes. For people with diabetes, the minimal protection provided by flip-flops increases the risk of cuts, blisters, and infections due to decreased sensation and poor wound healing. Additionally, the flat design offers little or no arch support, leading to pain and discomfort in the feet and ankles. If you have foot pain as a result of wearing flip-flops, it is suggested that you consult a podiatrist who can offer you relief tips, in addition to guiding you on more favorable footwear choices.
Flip-flops, though convenient, can be harsh on your feet, especially for individuals at risk like those with diabetes. The lack of support in flip-flops leads to improper heel strike, causing stress on the heels and increasing the risk of plantar fasciitis. Further, to keep the flip flops on, wearers often grip with their toes, which can cause muscle strain and negatively affect conditions like hammertoes. For people with diabetes, the minimal protection provided by flip-flops increases the risk of cuts, blisters, and infections due to decreased sensation and poor wound healing. Additionally, the flat design offers little or no arch support, leading to pain and discomfort in the feet and ankles. If you have foot pain as a result of wearing flip-flops, it is suggested that you consult a podiatrist who can offer you relief tips, in addition to guiding you on more favorable footwear choices.
Flip-flops are not always the best choice of footwear. If you have any concerns about your feet or ankles, contact John McGhan, DPM from Gold Canyon Foot & Ankle. Our doctor will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
When the weather starts warming up, people enjoy wearing flip-flops. Flip-flops are comfortable, stylish, and easy to slip on and off; they're perfect for any summer beach goer. However, these shoes can cause harm to the feet.
How Can Flip-Flops Affect Me Long-Term?
- Ankle problems
- Hip problems
- Lower back problems
- Pain in the balls of the feet
- Problems with foot arches
- Changes in the way you walk
Are There Injuries Associated with Flip-Flops?
Yes. Since flip-flops are relatively weak and do not provide the same amount of support as sneakers, people who wear flip-flops regularly are more susceptible to injuries. On top of that, the open nature of the shoe makes your feet more prone to other problems, such as cuts and even infections. Common injuries and ailments include:
- Sprained ankles
- Blisters
- Infections
- Cuts and Scrapes
I like Wearing Flip-Flops. Are There Safe Alternatives?
When buying flip-flops, try to find ones that have sturdy soles and that are made of high-quality materials that will support for your feet. These flip-flops will cost more but will also last longer as a result.
If you have any questions please feel free to contact our office located in Gold Canyon, AZ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flip Flops and Your Feet
When the weather heats up, you may want to start wearing flip-flops. However, it has been proven that these are not the ideal shoes in terms of preserving the health of your feet.
Flip flops are known to expose your feet to different types of bacteria and fungal infections. When you wear your flip flops in public, you are exposing them to staphylococcus which is a skin-irritating bacterium. Athlete’s foot is also highly contagious and can be spread when you walk around nearly-barefoot.
Another harmful effect of wearing flip-flops is that they develop blisters on the feet. This is because the thin strap rubs against the skin with each step taken. Unfortunately, when blisters pop, they cause you to be more vulnerable to pathogens you pick up by having your feet exposed.
These shoes may also cause “shooting pains”. If you have flat feet, you need arch support to keep your knees, hips, and back in alignment. If you wear flat shoes, your joints are forced to compensate which can cause injuries throughout the body.
If you constantly wear flip-flops, you should avoid doing so as they can lead to many problems for your feet. If you are experiencing any of these foot issues, you should seek help from a podiatrist right away.
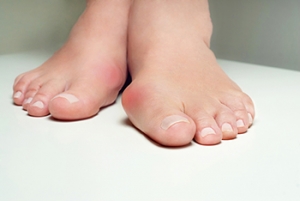
Symptoms and Causes of Bunions
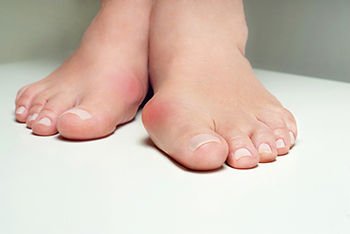
Bunions are bony bumps that form at the base of the big toe, causing it to deviate toward the other toes. This misalignment can lead to pain, swelling, and redness surrounding the joint. Symptoms often include a pronounced bump on the side of the foot, discomfort while walking, and restricted movement of the big toe. Bunions are typically caused by inherited foot structure abnormalities, but they can also result from or made worse by wearing tight or ill-fitting shoes that compress the toes. High heels and narrow-toed shoes are common culprits. Other contributing factors include arthritis and prolonged pressure on the feet. Early intervention with proper footwear, orthotic devices, and, in severe cases, surgery can alleviate symptoms and prevent further progression. A bunion can be painful and unsightly. If you have developed this foot condition, it is suggested that you visit a podiatrist who can offer you appropriate relief treatment methods.
If you are suffering from bunions, contact John McGhan, DPM of Gold Canyon Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Gold Canyon, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
Definition and Causes of Foot Stress Fractures
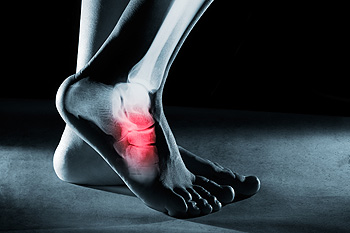
A foot stress fracture is a small crack or severe bruising within a bone, often resulting from repetitive force or overuse rather than a single traumatic event. Common causes include high-impact sports, sudden increases in physical activity, and wearing inadequate footwear. Stress fractures frequently occur in the weight-bearing bones of the foot, such as the metatarsals. Symptoms include pain that worsens with activity and diminishes with rest, swelling, and tenderness at the fracture site. Recovery time for a foot stress fracture typically ranges from six to eight weeks, depending on the severity and adherence to treatment. Proper rest, wearing supportive footwear, and gradually returning to activities are essential for healing. In some cases, immobilization with a boot or crutches may be necessary. If your foot hurts, it is suggested that you visit a podiatrist who can accurately diagnose and treat stress fractures.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact John McGhan, DPM from Gold Canyon Foot & Ankle. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Gold Canyon, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.